 and Esser, M., Practical Fracture Treatment, 5th Edition, 2008, Sydney, Churchill Livingston. 
and Ring, D., Proximal Humerus Fractures, in Evidence-based orthopedics, Bhandari, M., Editor, 2012, BMJ Books, London, UK. and Garg, A., The epidemiology of proximal humeral fractures, Acta Orthop Scand, 2001, 72(4): p.365-371. and Caesar, B., Epidemiology of adult fractures: a review, Injury, 2006, 37(8): p.691-697. Refer to physio for advice and starting of mobilisation.Pain from the fracture and restriction of movement is usual for 2-3 weeks and will require regular, then analgesia as required.Usually should start gradual mobilisation at 2 weeks. Sling required for 2-4 weeks depending on the patient and fracture.Other complications include nonunion and impingement from avulsed fracture fragments. The risk of developing diminished range of motion is more likely to occur in patients who do not perform range of motion exercises during recovery.Īlthough osteonecrosis of the humeral head is not common (7.9%), it can occur in patients with complex two, three and four-part fractures, especially in fractures involving the anatomic neck or severely displaced fractures. frozen shoulder), in which shoulder movement is painful and limited in all orientations. The decrease in motion ranges from clinically insignificant to adhesive capsulitis (i.e. Loss of shoulder mobility is among the more common complications of proximal humerus fractures. Secure in position of most comfort for the patient.Orthopaedic outpatient follow-up in 3-4 days 13 One-part fractures are almost always treated conservatively 8,9 Minimal trauma fracture in patients >50 years, arrange bone health assessment (i.e.12 Urgent orthopaedic referral is indicated for all nerve and vascular injuries, open fractures, and fracture dislocations. 11 Further indications for referral include fracture-dislocations and joint instability. Surgical intervention is generally needed for significantly displaced multi-part fractures and thus all displaced fractures should be referred to an orthopaedic surgeon for evaluation. 3 ED Management Optionsįor the majority of one-part fractures, these can be managed conservatively: analgesia, sling/sling and swathe and range of motion exercises. 10 However, while CT imaging improves the reliability of fracture classification over radiographs alone, however there is no evidence that CT improves outcome. Additional CT imaging is recommended if fracture lines cannot be reliably detected, as seen in complex three and four-part fractures with multiple-fragmented involvement of the head and tuberosities. Standard imaging studies of proximal humeral fractures consist of true anterior-posterior, outlet and axillary view. There is usually marked swelling, pain, tenderness and bruising of the proximal portion of the arm, due to bleeding from the bone and soft tissues. 8 However, this pattern has poor non-operative results, and as the articular surface is no longer attached to any parts of the humerus which are attached to soft tissues, it has a high incidence of osteonecrosis. Four-part fracture: These fractures are uncommon.Three-part fracture: These fractures account for approximately 5% of proximal humeral fractures.7 These fractures account for approximately 20% of proximal humeral fractures. Two-part fracture: Frequently seen in the setting of anterior shoulder dislocation.One-part fracture: These undisplaced/minimally displaced fractures account for over 70% of all proximal humeral fractures and are almost always treated conservatively.1 Most of these occur at home due to a fall, and in most cases they are an isolated injury. The majority of proximal humeral fractures occur in the elderly with ~70% occurring in women, presumably due to the greater incidence of osteoporosis. Source: Wikiradiography - Neck of Humerus Fractures Epidemiology Neer additionally defined two, three and four-part fractures to indicate the number of main segments affected by displacement see figure below. 3 ClassificationĪ “one-part” fracture is one in which the fragment is not displaced at all, or is displaced 45 degrees. 4 With regards to unstable fractures, surgical stabilisation may be required to achieve stability and pain relief, however this is not without its own risks. 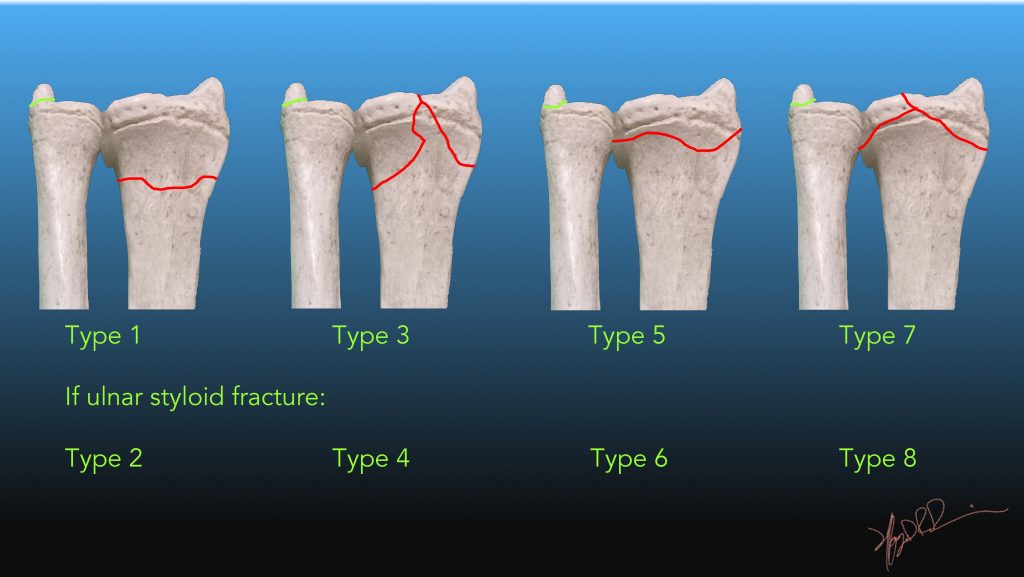
Physical therapies may be initiated after 3 weeks, making sure that no aggressive range-of-motion exercises, whether passive or actively assisted occurs until bony union has occurred. Gentle range-of-motion exercises can begin after 7-10 days in most stable fractures depending upon pain and tolerance.  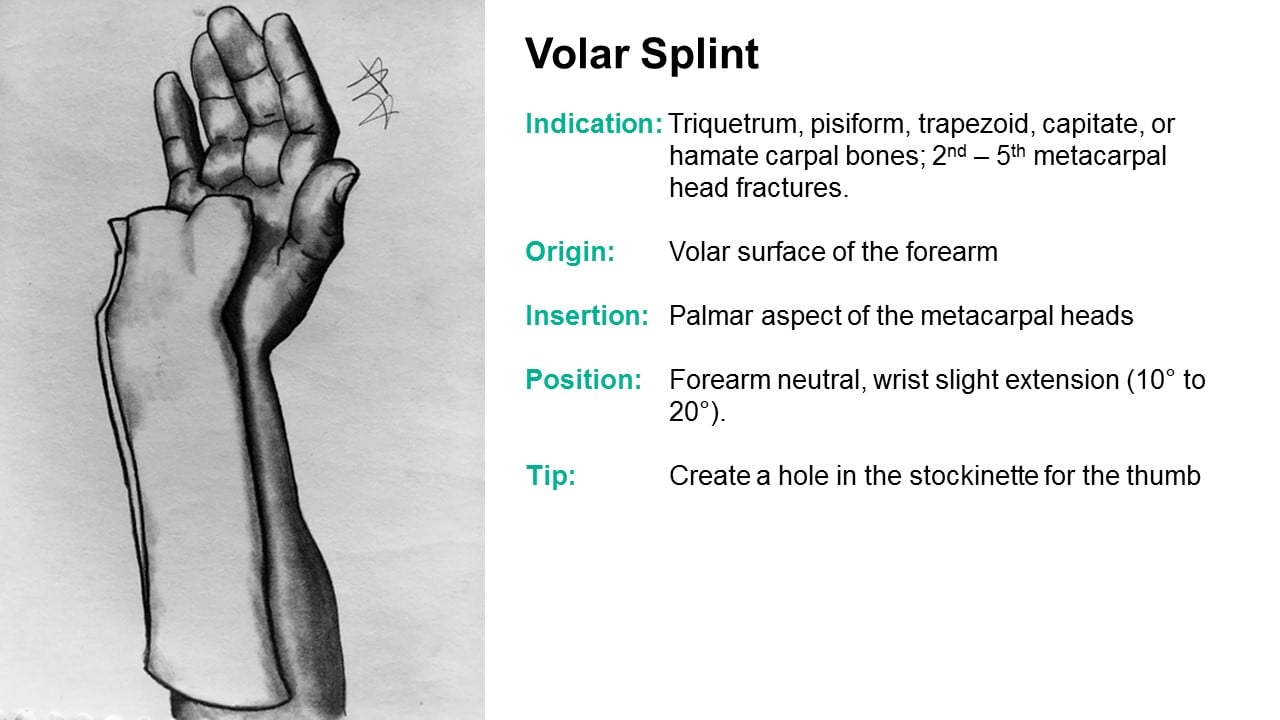
3 Immobilisation is achieved using either a sling, shoulder immobiliser or a splint, sling and swathe. 1, 2 Commonly non-displaced and often managed non-operatively using immobilisation methods. Commonly in the elderly and their incidence is increasing. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
